Lattice degeneration
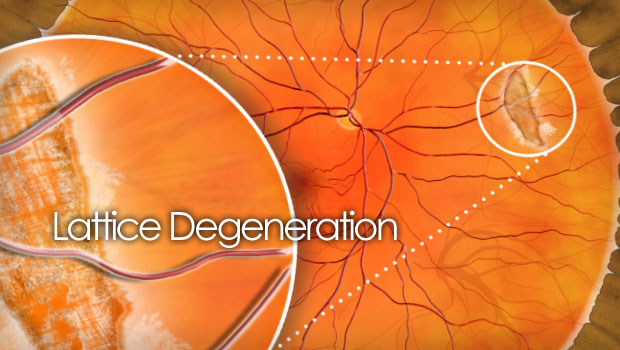

Lattice degeneration
Lattice degeneration is a retina condition in which the retinal tissue is abnormally thin and the blood vessels have a “lattice-like” appearance due to fibrosis.
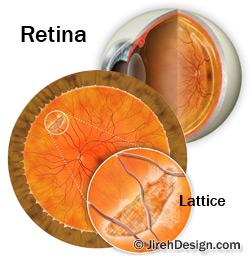
The typical lattice degeneration patient is over 25 years of age and may be myopic (nearsighted). It is typically found in both eyes. Estimates are that 8 to 11 percent of the population has peripheral retinal changes that are categorized as lattice degeneration.
Watch the “How vision works” animation
Lattice does not typically cause symptoms, but if symptoms occur, they include photopsia, or flashing lights in the patient’s peripheral (side) vision.
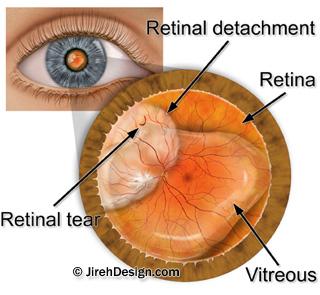
Lattice degeneration, along with vitreous detachment can be precursors to retinal detachment. Many vitreo-retinal physicians associate lattice with higher risk of retinal detachment. Retinal holes can occur in the lesions and tractional retinal tears can develop in rare cases.
Diagnosis of lattice degeneration is done by a well-dilated, peripheral retina examination called ophthalmoscopy. During ophthalmoscopy, the doctor sometimes uses scleral depression – a technique in which she applies slight pressure on the outside of the eye in order to give the her a better view of the peripheral retina.
Misdiagnosis of Lattice degeneration is not uncommon. If there are any suspicions of possible lattice, the vitreo-retinal specialist will do a dilated peripheral retinal exam. Regular dilated eye exams to detect and treat any possible complications are a good idea for the symptomatic patient.
An optometrist or ophthalmologist can monitor lattice degeneration but a vitreo-retina specialist will usually perform the treatment.
We are accepting new patients. If you think you may have symptoms of lattice degeneration, call The Macula Center at 727-789-8770.